
The future is virtual, especially for older people. Health economist Jane Sarasohn-Kahn explores how the industry is seeking out ways to serve older adults at home, especially in the midst of the coronavirus.
By Jane Sarasohn-Kahn, MA, MHSA
The COVID-19 pandemic revealed many weaknesses and gaps in U.S. health and social care. One among these adversely impacted older Americans beyond the coronavirus itself: the need for digital connectivity.
Without the ability to connect via broadband, older adults, many of whom were already isolated before the public health crisis, experienced further social isolation from family, friends, the community and medical providers. In the U.S., the growth of solo elders and “elder orphans,” older people living alone without a spouse or children on whom they can depend for caregiving, is a growing risk for both depression and poor chronic health management.
In the initial months of the pandemic, medical providers compelled patients to use virtual health programs for encounters in order to keep the virus at bay for their staff and for consumers to avoid potential exposure to COVID-19 in doctors’ offices and hospital clinics.
The opportunities for solving this challenge are addressed in The Future of Remote Care Technology and Older Adults: Connection is Everything, the latest report from Laurie Orlov, principal analyst for technology market research at Aging and Health Technology Watch.
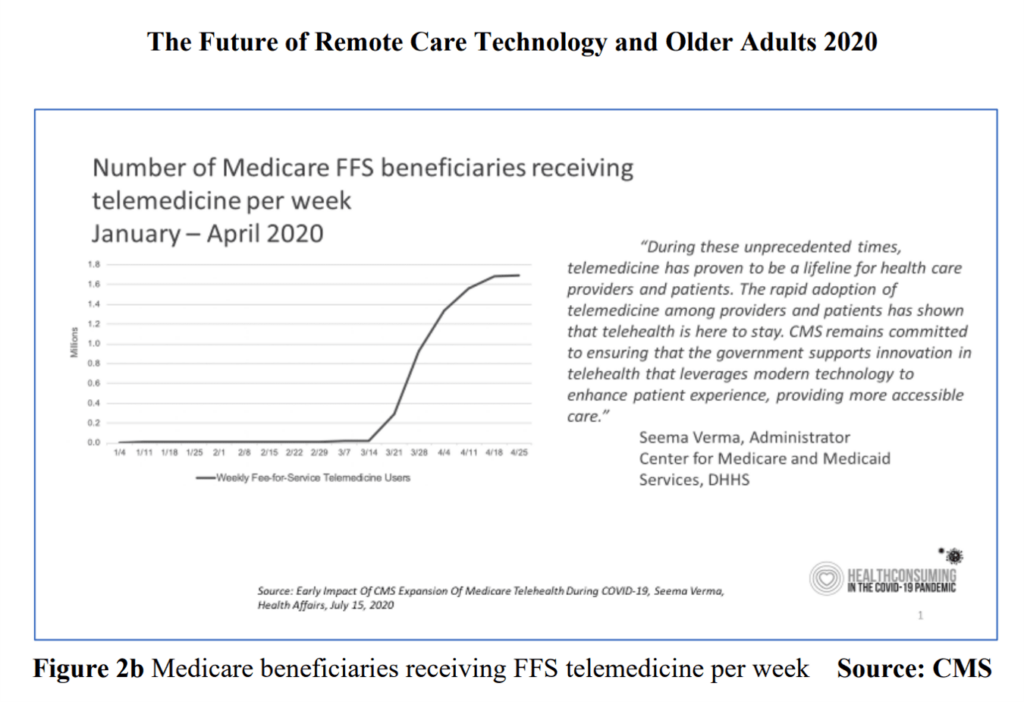
In the initial months of the pandemic, ad-hoc connections between patients and clinicians were made, via Wi-Fi hot spots and cellular linkups, Google Meetings and Zoom, and FaceTime phone calls. “For those communities with weak or no Wi-Fi, true creativity and/or new tools were required,” Orlov observed.
By the last week of April 2020, over 1.6 million fee-for-service telemedicine visits served Medicare enrollees, motivating Seema Verma, administrator of the Centers for Medicare & Medicaid Services (CMS) to say, “During these unprecedented times, telemedicine has proven to be a lifeline for health care providers and patients.”
CMS quickly adapted rules to enable more telehealth visits, along with establishing payments and pay the same rate for virtual care as for in-person visits.
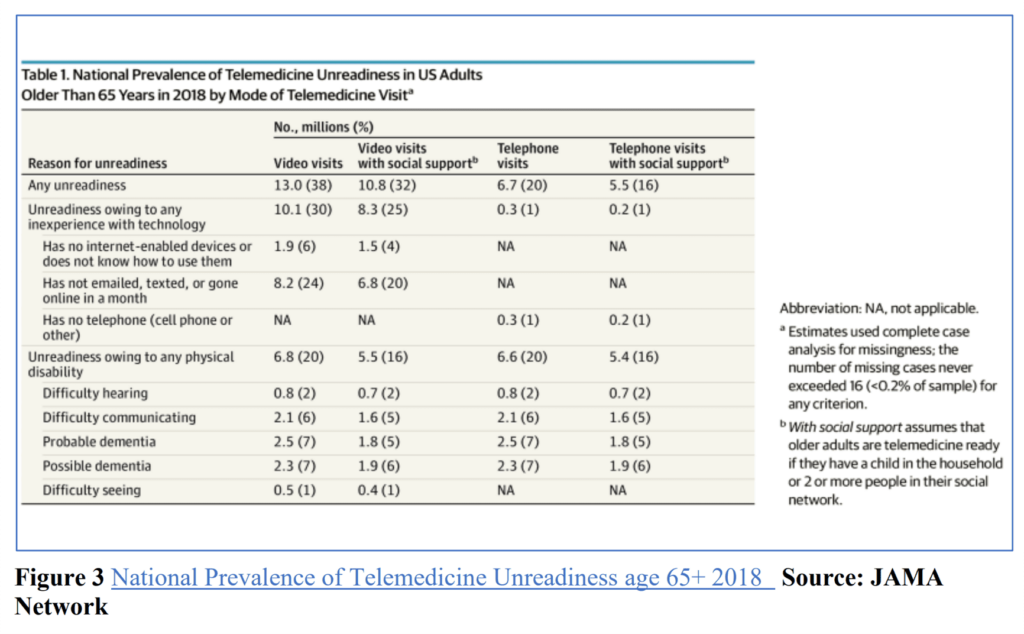
While CMS did its part to foster the telehealth supply side for providers to pivot to virtual care offerings, on the consumer demand side, the pandemic experience uncovered “telemedicine unreadiness,” illustrated in the table above with data from a recent JAMA study. Among people 65 years of age and older, major obstacles to being “ready” for telemedicine included inexperience with technology, such as not emailing, texting or going online, or not knowing how to use internet-enabled devices; and inexperience owing to physical disability, especially dementia or difficulty communicating.
Even with these potential limitations, technology developers and healthcare providers provided many creative options to connect older disconnected health consumers, including:
- Leveraging televisions, which seniors likely owned in their homes: For example, Independa provides connectivity through its SmartTV product, and MedSign enables “Talk to the Doctor” virtual care encounters
- Using voice tech digital assistants like Amazon Alexa to conduct ongoing check-in “calls” with people who may be isolated
- Adapting FaceTime and Skype-type calls with older people in lieu of commercially available telemedicine platforms
“For telehealth, the overwhelming news is video visits—the doctor’s office in your living room,” Dr. Joseph Kvedar, president of the American Telemedicine Association, told Orlov in the report.
Most people over 65 years of age who experienced a virtual care visit during the first six months of the pandemic appreciated the convenience, accessibility and care received in the encounter.
In its study on telehealth use among older adults before and during COVID-19, the University of Michigan’s National Poll on Healthy Aging found that:
- For a one-time follow-up visit after a medical procedure or surgery, interest in a telehealth visit rose from 55% in May 2019 to 63% in June 2020.
- For a visit with a provider whom they had previously seen, interest in a telehealth visit rose from 58% in May 2019 to 72% in June 2020.
- For a new patient visit or to discuss a new health problem, interest in a telehealth visit was similar in May 2019 (34%) and June 2020 (36%).
While it is still too early to fully understand the impacts of telehealth in the COVID-19 era, the experience on both the provider-supply side and consumer/patient-demand side has yielded lessons to build on. One key learning is that there are many pieces to the remote care technology “puzzle” and use cases beyond the “video visits” Dr. Kvedar noted.
There are rising expectations for remote care technology across all patient groups, but the opportunity to serve older people at home is particularly impactful given the virus’ impact on seniors’ limited access to face-to-face healthcare during the pandemic.
Virtual-first options are evolving in pioneering Medicare programs. Chatbots and portals are becoming more personalized and better designed, integrating with electronic health records systems including direct connections to telehealth appointments. Artificial intelligence (AI), robotics and machine learning capabilities are becoming part of remote care, Orlov notes, quoting Ashutosh Saxena, CEO of Caspar.AI, who told her: “Using AI, Caspar makes a behavior model from sensor data, deriving 50 sets of analytics like sleep quality, activity levels, changes in behavior patterns. Caspar uses these wellness analytics to motivate [people] to move more.”
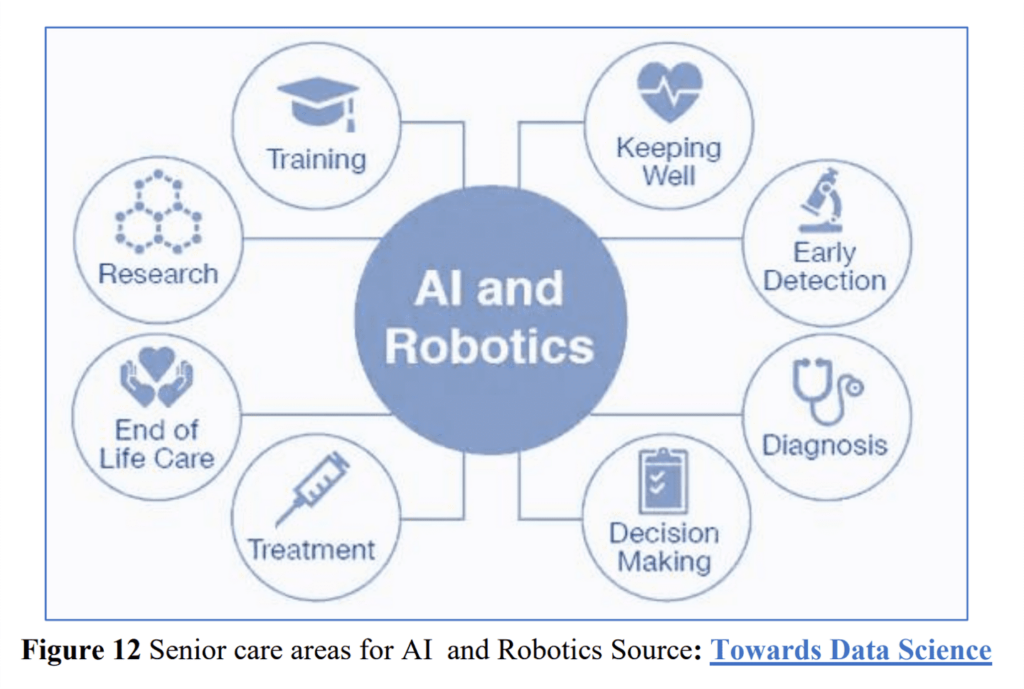
In fact, AI and robotics are getting embedded across the continuum of care as shown in this diagram. The home care provider Home Instead collaborates with GrandPad to personalize care for clients, embedding their tablet with data and underlying analytics placed in the hands of home health workers.
“In the future, we see care plans remotely delivered in tablet format along with voice-enabled discharge instructions,” Rob Flippo, CEO of MobileHelp, told Orlov. This is part of the vision of the home becoming the hub for life and care, which will be enabled through wearables with alerts, peer-to-peer health and care networking, and real-time agents trained in social work for the payer-provider market—providing access to more than a typical call-center conversation, David Inns, CEO of GreatCall, envisions.
While we are still in the midst of battling the coronavirus, which is hitting older people in America especially hard, Orlov’s report gives us a hopeful road map to rebuilding care in a better, safer, more cost-effective and humane setting: our homes. Many building blocks of the technologies and applications are available now, and analytics and virtual reality and augmented reality are evolving, spurred on by the public-health crisis. May we work together across the healthcare ecosystem to close the gaps in this vision—connectivity, public policy and training—and raise up the new care paradigm that older health citizens deserve.



About The Author: Jane Sarasohn-Kahn, MA, MHSA
Through the lens of a health economist, Jane defines health broadly, working with organizations at the intersection of consumers, technology, health and healthcare. For over two decades, Jane has advised every industry that touches health including providers, payers, technology, pharmaceutical and life science, consumer goods, food, foundations and public sector.
More posts by Jane Sarasohn-Kahn, MA, MHSA